Everest Base Camp altitude sickness prevention starts with understanding the thin air. Oxygen levels drop significantly as you climb higher into the Himalayas. Trekkers often feel headaches, fatigue, and shortness of breath during the climb. Poor sleep and physical stress make these symptoms worse. High-quality trekking conditions provide the support needed for a safer climb. Better rest and professional care help the body adjust to the high elevation.
Everest Base Camp altitude sickness prevention depends on a slow ascent, proper acclimatization, 3 to 4 liters of fluids daily, warm layers, regular meals, and immediate descent if symptoms worsen. Most trekkers need acclimatization days in Namche Bazaar and Dingboche to adjust safely.
The ascent to the foot of the world’s highest peak represents one of the most profound physiological challenges accessible to non-professional mountaineers. As individuals navigate the rugged terrain of Nepal’s Khumbu region, their bodies are continually subjected to a relentless state of hypobaric hypoxia. This condition, characterized by a lower partial pressure of oxygen in the inspired air due to decreased atmospheric pressure, forces rapid and exhaustive physiological adaptations.
The human biological machine must rapidly alter its ventilatory rate, cardiovascular output, and eventually its hematopoietic processes just to maintain baseline cellular function. When these adaptive mechanisms fall behind the rate of ascent, altitude sickness manifests, threatening not only the success of the expedition but the life of the trekker. In this extreme environment, logistical support for the climber ceases to be a mere luxury and becomes a critical factor in medical safety.
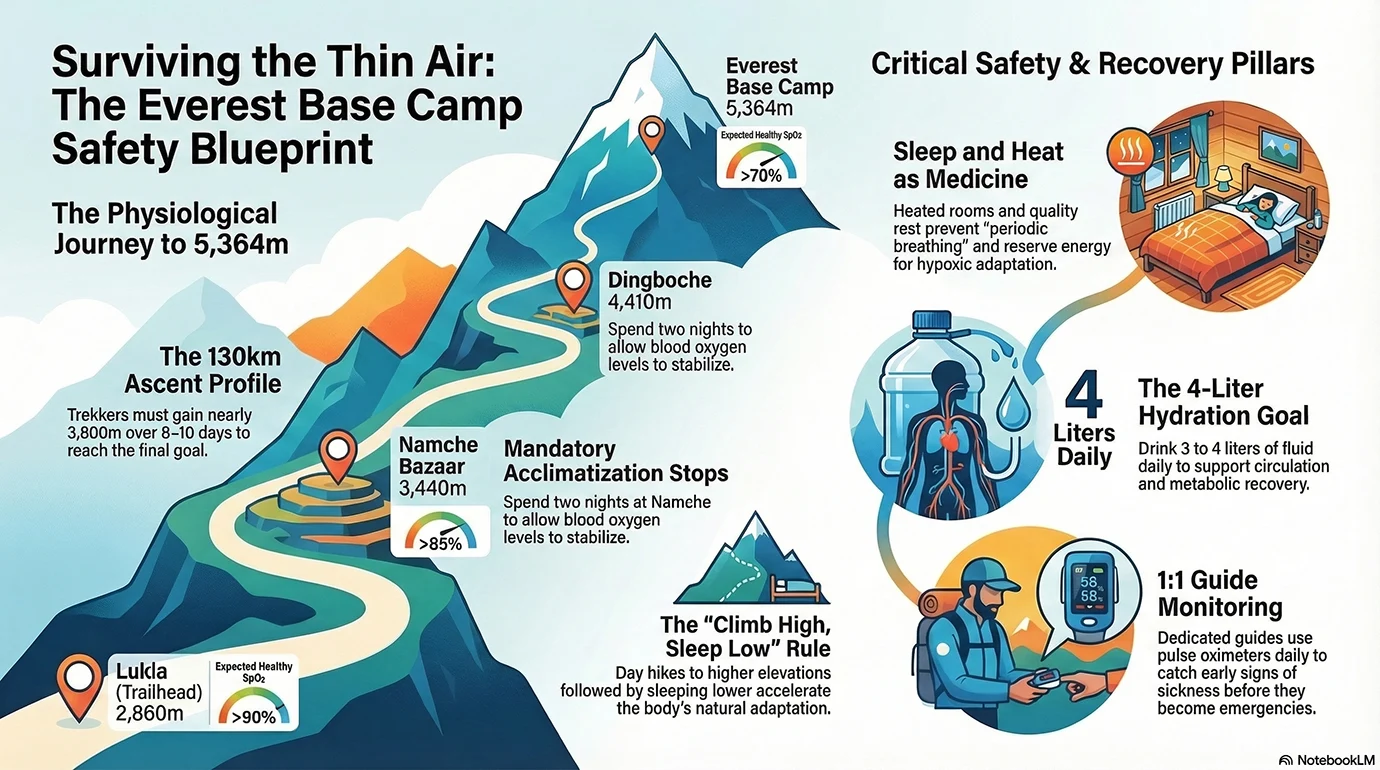
Luxury trekking models profoundly alter the expedition’s physiological baseline by neutralizing secondary environmental stressors, ensuring that the trekker’s physiological reserves are devoted entirely to hypoxic adaptation rather than to battling cold, malnutrition, or sleep deprivation.
Quick Facts
- Main Risk: Acute Mountain Sickness above 3,000 m
- EBC Altitude: 5,364 m / 17,598 ft
- Best Prevention: Slow ascent with acclimatization days
- Daily Water Goal: 3 to 4 liters
- Emergency Rule: Stop, rest, and descend if symptoms worsen
Medical Disclaimer: This article shares general information about Everest Base Camp altitude sickness prevention and does not replace medical advice. Consult your doctor before high-altitude travel, especially if you have heart, lung, or blood pressure conditions.
What Causes Altitude Sickness on the Everest Base Camp Trek
At altitudes above 3,000 meters, air pressure drops, so each breath delivers the body less oxygen. On the Everest Base Camp trek, the oxygen percentage in the air stays the same, but the air pressure falls fast as you go higher. Everest Base Camp altitude sickness prevention starts with understanding this change and giving the body time to adjust.
When oxygen levels drop, the body breathes faster, and the heart works harder. Over a few days, the body also makes more red blood cells to better carry oxygen. If you climb too fast, the body cannot keep up, and symptoms such as headache, fatigue, dizziness, and shortness of breath can develop.
Cold weather, dehydration, poor food, and physical exhaustion make the problem worse. Everest Base Camp altitude sickness prevention does not depend on fitness alone, because even strong trekkers can get sick at high altitude. A slow pace, proper acclimatization, warm clothing, enough water, and good rest help lower the risk.
Everest Base Camp Altitude Profile
Understanding the elevation helps plan a safe route. Lukla sits at about 2,860 m. Namche Bazaar reaches about 3,440 m. Dingboche stays around 4,410 m. Lobuche rises to about 4,940 m. Everest Base Camp reaches the final goal of 5,364 m. Air becomes significantly thinner at each stage. Slow movement becomes vital as the altitude at Everest Base Camp increases.
The Everest Base Camp trek spans approximately 130 kilometers (65 kilometers each way) and requires trekkers to gain nearly 3,800 meters in elevation over 8 to 10 days of ascent. Analyzing the topographical steps of this trek is essential for anticipating physiological bottlenecks and executing targeted safety interventions.
| Location | Approximate Elevation (Meters) | Approximate Elevation (Feet) | Expected Arterial SpO2 Healthy Range |
|---|---|---|---|
| Kathmandu (Pre-trek) | 1,350 m | 4,429 ft | >93% |
| Lukla (Trailhead) | 2,840 m – 2,860 m | 9,317 ft – 9,383 ft | >90% |
| Phakding | 2,610 m | 8,562 ft | >90% |
| Namche Bazaar | 3,440 m | 11,286 ft | >85% |
| Tengboche / Deboche | 3,710 m – 3,860 m | 12,171 ft – 12,664 ft | >80% |
| Dingboche | 4,410 m | 14,468 ft | >75% |
| Lobuche | 4,910 m – 4,940 m | 16,108 ft – 16,207 ft | >72% |
| Gorak Shep | 5,164 m | 16,942 ft | ~70% |
| Everest Base Camp | 5,364 m | 17,598 ft | >70% |
| Kala Patthar | 5,545 m – 5,644 m | 18,192 ft – 18,517 ft | <70% |
The trek typically commences with a dramatic flight from Kathmandu to the Tenzing-Hillary Airport in Lukla. Arriving at an altitude where atmospheric pressure is already significantly compromised, trekkers immediately enter the preliminary stages of hypoxic exposure. To ease the transition, the first day involves a gradual descent to the village of Phakding at 2,610 meters, allowing the body to recover from the initial altitude shock.
The second day initiates the true upward trajectory, climbing steeply through pine forests and crossing high suspension bridges to reach Namche Bazaar. Namche is the undisputed commercial and cultural capital of the Sherpa region, sitting in a natural amphitheater at 3,440 meters. It serves as the first mandatory physiological checkpoint. Because the ascent from Phakding exceeds the recommended daily sleeping elevation gain limit of 500 meters, trekkers universally spend two nights here to allow their respiratory and hematopoietic systems to catch up.
Following the Namche acclimatization phase, the trail continues deeper into the alpine environment. Trekkers pass through the spiritual center of Tengboche (or the slightly lower, more sheltered Deboche) at approximately 3,860 meters, before continuing above the tree line to Dingboche. Situated at 4,410 meters in the arid Imja Valley, Dingboche represents the transition into extreme altitude. The lack of vegetation and the drastic drop in oxygen saturation (typically hovering around 75%) dictate a second mandatory acclimatization day. Here, physiological strain is palpable; resting heart rates remain elevated, and the simple act of walking to a dining hall induces breathlessness.
The final pushes are grueling. The trail winds through the glacial moraine of the Khumbu Glacier to Lobuche at 4,940 meters, where the physiological margin of safety becomes perilously thin. From Lobuche, trekkers move to the final outpost of Gorak Shep at 5,164 meters, navigating rocky, uneven terrain before making the triumphant but exhausting march to Everest Base Camp at 5,364 meters.
Many itineraries also include an early morning ascent of Kala Patthar, a rocky vantage point at 5,644 meters that offers the most iconic, unobstructed views of Mount Everest. At these terminal elevations, ambient oxygen availability is critically low, and maintaining a slow, deliberate pace is no longer a recommendation—it is a strict biological imperative to avoid collapsing from high-altitude pulmonary or cerebral edema.

Everest Base Camp Altitude Sickness Prevention Basics
Everest Base Camp altitude sickness prevention starts with a slow and steady ascent. After 3,000 meters, trekkers should gradually acclimatize by spending nights at higher elevations, including acclimatization days in places like Namche Bazaar and Dingboche. Day hikes to a higher point, followed by sleep at a lower altitude, help the body adjust more safely.
Everest Base Camp altitude sickness prevention also depends on proper hydration and food. Trekkers should drink about three to four liters of water each day and add electrolytes when needed. High-calorie meals, especially foods rich in carbohydrates, help maintain energy and support the body at high altitude.
Warm clothing and good rest also play major roles in preventing altitude sickness at Everest Base Camp. Cold weather increases physical stress and makes acclimatization harder. Trekkers should sleep well, stay warm, and avoid alcohol, sleeping pills, and strenuous exercise, as these can reduce breathing efficiency and increase the risk of altitude sickness.
Why Luxury Treks Offer Better Safety at Altitude
While the physiological rules of high-altitude adaptation apply equally to all humans, the environments in which those adaptations occur vary widely depending on the chosen trekking logistical framework. Standard budget treks prioritize cost, meaning trekkers endure shared, unheated accommodations, basic meals, and high guide-to-client ratios. Conversely, luxury Everest Base Camp packages—often ranging from $3,500 to over $6,000—optimize for physiological support, comfort, and risk mitigation. By comprehensively minimizing secondary stressors such as cold exposure, malnutrition, and psychological anxiety, luxury treks fundamentally alter the safety equation, routinely achieving success rates that eclipse those of standard operations.

Better Sleep Supports Better Acclimatization
Heated rooms and comfortable beds provide deep rest. Proper sleep allows the heart and lungs to recover faster. Basic teahouses often feel freezing and damp. Luxury lodges keep trekkers warm and well-rested. Good sleep remains a key part of preventing altitude sickness at Everest Base Camp.
High-altitude sleep is notoriously fragile and inherently unrefreshing for the unacclimatized body. The primary culprit is a phenomenon known as periodic breathing, or Cheyne-Stokes respiration. In a hypoxic environment, the lack of oxygen stimulates the brain to command faster, deeper breathing. This hyperventilation successfully raises blood oxygen levels but concurrently blows off massive amounts of carbon dioxide, leading to hypocapnia.
Because carbon dioxide is the primary chemical trigger for the respiratory drive during sleep, the brain senses the low CO2 levels and temporarily halts breathing altogether (central apnea). The trekker stops breathing until oxygen levels plummet and carbon dioxide builds back up, triggering a sudden, gasping awakening. This cycle repeats endlessly throughout the night, completely destroying slow-wave (deep) sleep and leaving the cardiovascular system in a state of perpetual sympathetic arousal.
To survive and adapt, the body desperately needs uninterrupted periods of rest to repair microtrauma in the muscles and stabilize heart rate. Heated rooms and comfortable beds provide deep rest by removing the compounding stress of extreme cold. Proper sleep allows the heart and lungs to recover faster from the brutal exertion of the day. In stark contrast, basic teahouses often feel freezing and damp. Constructed with thin plywood walls and lacking central insulation, temperatures inside standard rooms frequently drop below freezing. Trekkers in these environments are forced to sleep in thick down jackets inside their sleeping bags, frequently waking up to urinate due to cold diuresis and braving icy, shared pit toilets.
Luxury lodges keep trekkers warm and well-rested. Accommodations like Yeti Mountain Home and Everest Summit Lodge offer a level of infrastructural comfort that actively supports acclimatization. Featuring en-suite bathrooms with hot showers, thick mattresses, fine linens, and critically, electric blankets or room heaters, these high-end lodges eliminate the shivering and thermal stress that plague standard treks. By providing a genuinely restorative environment where the body feels secure, good sleep remains a key part of Everest Base Camp altitude sickness prevention, ensuring the trekker wakes up with the physiological bandwidth required to face the next stage of the ascent.

Better Nutrition Helps the Body Adjust
Everest Base Camp altitude sickness prevention also depends on good food and clean cooking. At high altitude, many trekkers lose their appetite and feel mild nausea. Fresh meals, warm drinks, and regular eating times help the body maintain strength and adjust more easily to the thin air.
The body needs more energy in cold and high conditions, so balanced meals play a big role in recovery. Carbohydrate-rich foods help support energy, while soups, tea, and other warm fluids help with hydration and comfort. Better meal quality also helps trekkers eat enough, even when altitude reduces hunger.
Everest Base Camp altitude sickness prevention becomes harder when stomach problems start on the trail. Diarrhea or vomiting can cause fast dehydration and raise the risk of Acute Mountain Sickness. Clean kitchens, safe drinking water, and proper food handling reduce that risk and help trekkers stay stronger at high altitude.
1:1 Private Guide Ratio Improves Safety
A private guide watches every step. Close attention helps spot early signs of sickness. The guide can instantly change the walking pace. Personal support ensures the trek matches the individual’s physical needs.
The structural safety of an expedition is heavily dictated by the client-to-guide ratio. On standard, budget-focused treks, a single guide may be responsible for a group of 10 to 15 trekkers, supported by a handful of porters. In these scenarios, the guide’s attention is dangerously fragmented. They are forced to set an average group pace that may be too fast for the slowest members and too slow for the fastest, leading to suboptimal exertion profiles across the board. More alarmingly, a guide managing a large, dispersed group cannot continually monitor the nuanced physical deterioration of a single individual at the back of the pack.
Conversely, luxury treks operate on highly condensed ratios, typically providing one guide for every two to five trekkers, and frequently offering true 1:1 private guide support for those who demand the highest safety margins. A private guide watches every step, monitoring respiratory rates, gait changes, and subtle shifts in demeanor. Close attention helps spot early signs of sickness that a trekker might otherwise ignore. At high altitudes, cognitive impairment and the psychological desire to avoid disappointing the group often lead trekkers to hide their symptoms, dismissing a throbbing headache as a mere annoyance rather than a harbinger of cerebral edema. A dedicated guide is trained to pierce through this denial, conducting rigorous daily assessments.
Because they are not bound by the momentum of a large group, the guide can instantly change the walking pace. If a trekker demonstrates signs of excessive cardiovascular strain on the steep incline toward Tengboche, the private guide will immediately slow the pace, mandate a hydration break, or redistribute the trekker’s remaining pack weight to a porter. Personal support ensures the trek matches the individual’s physical needs, allowing for highly flexible itineraries in which an extra rest day can be seamlessly integrated into the schedule without disrupting the travel plans of a dozen strangers.

Daily Pulse Oximeter Checks Catch Problems Early
Guides check oxygen saturation and heart rates every day. Oxygen numbers show how well the body adjusts to the height. Daily monitoring helps guides make smart safety decisions. Early detection prevents minor issues from becoming dangerous.
Subjective self-reporting of symptoms is notoriously unreliable in hypoxic environments, making objective physiological data indispensable. On luxury treks, guides check oxygen saturation and heart rates every day using handheld finger pulse oximeters, typically recording these metrics both in the morning upon waking and in the evening after the day’s exertion. These small, non-invasive devices utilize red and infrared light absorption to measure the percentage of hemoglobin binding sites in the bloodstream occupied by oxygen ($SpO_2$).
Oxygen numbers indicate how well the body adjusts to high altitude, but they must be interpreted within the specific context of high-altitude medicine. At sea level, a healthy individual will display an $SpO_2$ between 97% and 100%; anything below 90% is considered a clinical emergency. However, on the Everest Base Camp trail, standard physiological parameters are entirely rewritten.
| Location | Altitude | Expected SpO2 Reading for Acclimatized Trekker |
|---|---|---|
| Lukla | 2,860 m | >90% |
| Namche Bazaar | 3,440 m | >85% |
| Tengboche | 3,860 m | >80% |
| Dingboche | 4,410 m | >75% |
| Lobuche | 4,940 m | >72% |
| Everest Base Camp | 5,364 m | >70% |
While a reading of 75% in Dingboche is considered a normal, healthy adaptation to the available atmospheric pressure, the pulse oximeter’s true value lies in tracking individual trends and identifying severe deviations from the expected baseline. If a trekker in Namche Bazaar registers an $SpO_2$ of 65% alongside a resting heart rate of 115 beats per minute, the guide immediately recognizes a critical failure in acclimatization, even if the trekker claims to feel relatively fine.
Daily monitoring helps guides make smart safety decisions, integrating oximetry data with the clinical Lake Louise Score questionnaire to form a complete medical picture. Early detection prevents minor issues from becoming dangerous. By identifying dangerous hypoxemia before fluid begins to pool in the lungs or brain, guides can preemptively enforce a rest day, administer prophylactic medications like Acetazolamide, or initiate a safe, controlled descent before a catastrophic medical evacuation becomes necessary.

Warm Lodges Reduce Physical Stress
Less cold exposure means the body uses less energy to stay warm. Warm environments lower physical fatigue. Recovery happens much faster in a comfortable setting. Staying warm is vital for preventing altitude sickness at Everest Base Camp.
The synergistic threat of hypoxia and extreme cold constitutes a severe challenge to human physiology. In lower temperatures, the body triggers peripheral vasoconstriction—narrowing the blood vessels in the skin and extremities to preserve core temperature. This defense mechanism significantly increases systemic vascular resistance, forcing the heart to pump harder and dramatically elevating blood pressure, adding severe mechanical strain to a cardiovascular system already working overtime due to oxygen deprivation.
Less cold exposure means the body uses less energy to stay warm. When temperatures plummet, the body initiates shivering thermogenesis, a highly energy-intensive process that rapidly depletes finite glycogen stores and increases cellular oxygen consumption, exacerbating the hypoxia the body is trying to combat. Luxury treks neutralize this threat through advanced infrastructural support. Warm environments lower physical fatigue by allowing the cardiovascular system to downregulate and the skeletal muscles to relax.
Furthermore, emerging sports science on cross-adaptation suggests that mitigating thermal stress leaves the body better able to handle hypoxic stress. Studies indicate that heat acclimation and maintaining a warm core temperature improve blood flow dynamics and oxygen delivery efficiency, providing an unexpected yet powerful buffer against altitude sickness.
Recovery happens much faster in a comfortable setting; the vasodilation induced by heated dining rooms, hot showers, and electric blankets facilitates the rapid clearance of lactic acid and metabolic waste products generated during the day’s grueling ascent. Ultimately, staying warm is vital for preventing altitude sickness at Everest Base Camp, as it shifts the body’s resources from sheer survival to active, efficient acclimatization.

Reliable Logistics and Emergency Support Matter
Preventing altitude sickness at Everest Base Camp depends on careful planning from the first day of the trek. In the remote Khumbu Valley, a well-managed itinerary gives trekkers time to rest, adjust, and recover if symptoms appear. Flexible schedules, smooth lodge arrangements, and expert logistics help keep the trek safe and reduce unnecessary stress.
Everest Base Camp altitude sickness prevention also depends on fast communication and reliable emergency support. Professional guides carry satellite phones, GPS devices, oxygen, and high-altitude medical supplies to respond quickly if problems develop. Strong evacuation planning, expert care, and close support give trekkers more confidence and help them focus on their health.
Signs of Altitude Sickness Every Trekker Should Know
Mild symptoms include slight headaches or loss of appetite. Moderate symptoms bring persistent vomiting or a nagging cough. Severe symptoms involve confusion or trouble walking. Stop the climb if symptoms appear. Rest or descend immediately if the condition gets worse. Safety always comes first on the mountain.
The clinical presentation of altitude sickness operates on a continuum, and recognizing the transition from benign physiological adaptation to pathological deterioration is paramount. Medical professionals and expedition guides rely heavily on the Lake Louise Scoring System, which quantifies the severity of AMS based on self-reported headache, gastrointestinal symptoms, fatigue/weakness, and dizziness/lightheadness.
Mild symptoms include slight headaches or loss of appetite, often accompanied by unusual fatigue, mild dizziness upon standing, and difficulty sleeping. These warning signs are incredibly common, frequently appearing within 2 to 12 hours after arriving at a new altitude. Crucially, mild AMS is highly manageable. The standard protocol dictates that the trekker must halt their ascent and rest at their current elevation, maintaining hydration and caloric intake until the symptoms resolve, which typically occurs within 24 to 48 hours.
Moderate symptoms bring persistent vomiting or a nagging cough, signaling that the body is losing the battle against hypoxia. A severe headache that does not respond to standard over-the-counter analgesics like ibuprofen or paracetamol, coupled with extreme lethargy that makes moving from the bed difficult, indicates a dangerous escalation. If a dry, persistent cough develops alongside shortness of breath at rest, the pulmonary capillaries may be beginning to leak fluid.
Severe symptoms involve confusion or trouble walking, indicating the onset of the lethal variants of altitude illness: High-Altitude Cerebral Edema (HACE) and High-Altitude Pulmonary Edema (HAPE). HACE is characterized by severe ataxia (the inability to walk in a straight line), profound disorientation, hallucinations, slurred speech, and eventually a lapse into a coma as fluid crushes the brain against the skull. HAPE manifests as a suffocating tightness in the chest, extreme breathlessness even while completely inactive, a gurgling sound during breathing, cyanosis (blue or gray lips and fingernails), and coughing up pink, frothy sputum.
Stop the climb if symptoms appear. The golden rule of mountaineering states that any illness at altitude is altitude sickness until proven otherwise, and one must never ascend with worsening symptoms. Rest or descend immediately if the condition gets worse. Descent is the definitive, ultimate cure for all forms of altitude sickness. Dropping just 500 to 1,000 meters in elevation can drastically increase the partial pressure of oxygen and reverse life-threatening symptoms within hours.
If descent is impossible due to weather or terrain, the immediate administration of supplemental oxygen, pharmaceutical interventions, or the use of a portable hyperbaric chamber is required. Safety always comes first on the mountain; a delayed summit or an aborted trek is infinitely preferable to a fatal case of edema.
Daily Habits That Lower AMS Risk on the Trek
Everest Base Camp altitude sickness prevention depends on steady daily habits from the first day of the trek. Walk at a slow, even pace so the body has time to adjust to the rising altitude. Sip water throughout the day rather than waiting until you feel thirsty. Eat regular meals and snacks even when your appetite drops, because the body needs fuel to adapt and recover. Stay warm with proper layers, especially during rest stops and cold evenings. Tell your guide about any headache, nausea, dizziness, or unusual fatigue as soon as it starts. Use every acclimatization day to the fullest, because those rest days help the body catch up and reduce the risk of serious altitude-related problems.
Common Mistakes That Increase Altitude Risk
Everest Base Camp altitude sickness prevention depends on avoiding common mistakes that raise risk on the trail. Walking too fast puts extra stress on the body and reduces the time needed for safe acclimatization. Ignoring a headache or other early symptoms can allow altitude sickness to worsen quickly. Skipping rest days makes it harder for the body to adjust to the altitude at Everest Base Camp, while poor hydration reduces energy and limits proper oxygen use.
Low-quality lodges, weak meals, cold rooms, and limited guide support also make recovery harder. Trekkers who follow a steady pace, take acclimatization seriously, drink enough water, and choose strong support systems give themselves a much better chance of reaching Everest Base Camp safely.
Who Benefits Most from a Luxury Everest Base Camp Trek
Everest Base Camp altitude sickness prevention becomes much easier on a Luxury Everest Base Camp Trek because premium support improves both safety and recovery. First-time trekkers gain confidence from close guide supervision and a well-managed pace. Older travelers rest better in warm, comfortable lodges and benefit from a slower ascent plan. Families and couples enjoy more privacy, better rooms, and a calmer trekking experience. Travelers who care about strong safety standards often choose premium options because expert guides, better accommodations, and reliable logistics create a safer and more comfortable path to Everest Base Camp.

Why a Luxury Everest Base Camp Trek Gives More Confidence
Everest Base Camp altitude sickness prevention improves when trekkers stay in upgraded lodges, follow a structured acclimatization plan, and receive close guide support each day. Warm rooms, hot meals, and better rest help the body recover faster in cold and high conditions.
Expert guides manage pace, watch symptoms, and make smart decisions before small problems grow. Daily health checks, including pulse oximeter monitoring, add another layer of safety and give trekkers more confidence on the trail. Strong logistics, reliable emergency backup, and steady support all work together to reduce stress and improve the chance of reaching Everest Base Camp safely and comfortably.
Practical Tips Before You Go
Start light cardio training a few months before the trek. Use stairs, hills, or long walks to build leg strength and improve endurance. Everest Base Camp altitude sickness prevention starts before arrival in Nepal, not on the trail. A doctor should review your health, advise on altitude medicine if needed, and help you prepare for high altitude travel. Pack your regular medications, warm layers, and gear to keep you dry and comfortable. Travel insurance should cover high-altitude trekking and helicopter evacuation. Good preparation lowers risk, supports acclimatization, and makes the trek safer and smoother.
| Medication | Primary Use | Standard Altitude Dosage | Mechanism / Notes |
|---|---|---|---|
| Acetazolamide (Diamox) | AMS Prevention / Acclimatization | 125 mg every 12 hours | Stimulates respiration; increases oxygenation |
| Dexamethasone | Emergency Treatment (HACE/AMS) | 4 mg every 6 hours | Potent steroid; reduces brain swelling |
| Nifedipine | Emergency Treatment (HAPE) | Varies (consult physician) | Lowers pulmonary artery pressure |
| Tadalafil | HAPE Prevention / Treatment | 10 mg twice daily | Phosphodiesterase-5 inhibitor; lowers pulmonary pressure |
Pack personal medications and warm clothing. A comprehensive medical kit should include ibuprofen, paracetamol, loperamide (for diarrhea), oral rehydration salts, throat lozenges, and broad-spectrum antibiotics. Gear selection is critical; invest in a high-quality, windproof Gore-Tex outer shell, thermal base layers, an insulated down jacket, and a sleeping bag rated to at least -10°C (even if staying in luxury lodges, as extreme weather is unpredictable).
Finally, ensure travel insurance covers helicopter evacuation. This is arguably the most critical administrative step of the preparation process. Standard travel insurance policies explicitly exclude high-altitude mountaineering and helicopter extractions. Trekkers must purchase specialized policies that cover emergency medical evacuation up to 6,000 meters. A helicopter rescue from Dingboche can cost thousands of dollars, and lacking proper insurance can fatally delay an extraction. Staying prepared makes the trek much smoother, effectively neutralizing logistical anxieties so the trekker can focus entirely on the physical and spiritual trek ahead.
Conclusion
Everest Base Camp altitude sickness prevention relies on careful preparation, a slow ascent, proper rest, good food, and strong guide support. Trekkers need time to adjust to thin air, and even small mistakes at high altitude can raise the risk of serious illness. A skilled guide helps manage pace, checks health signs, and acts quickly if symptoms worsen. Luxury trekking conditions add another layer of safety because warm rooms, better sleep, nutritious meals, and reliable emergency planning help the body adapt more effectively. For travelers seeking greater safety, comfort, and a higher chance of completing the trek successfully, a luxury option offers one of the smartest approaches to preventing altitude sickness at Everest Base Camp.
FAQs About Everest Base Camp Altitude Sickness Prevention
1. What is altitude sickness on the Everest Base Camp trek?
Altitude sickness occurs when your body cannot adjust quickly enough to the lower oxygen levels at high altitude. On the Everest Base Camp trek, it often starts with headache, fatigue, dizziness, nausea, or poor sleep.
2. At what altitude does altitude sickness start on the Everest Base Camp trek?
Altitude sickness can start above 3,000 meters. Many trekkers notice symptoms after Namche Bazaar, and the risk rises further in Dingboche, Lobuche, and Gorak Shep.
3. How can I prevent altitude sickness at Everest Base Camp?
Everest Base Camp altitude sickness prevention depends on a slow ascent, enough rest days, good hydration, warm clothing, regular meals, and honest communication with your guide. A rushed climb raises the risk.
4. How many acclimatization days do I need for Everest Base Camp?
Most safe itineraries include at least two acclimatization days, usually in Namche Bazaar and Dingboche. These stops help your body adjust before you move to the next level.
5. What are the first signs of altitude sickness at Everest Base Camp?
The first signs usually include headache, loss of appetite, unusual tiredness, mild nausea, dizziness, and poor sleep. These symptoms often appear before more serious problems develop.
6. Can fit trekkers still get altitude sickness on the Everest Base Camp trek?
Yes. Fitness does not protect you from altitude sickness. Strong trekkers often walk too fast, which can actually increase the risk.
7. How much water should I drink to prevent altitude sickness at Everest Base Camp?
Most trekkers should drink about 3 to 4 liters of fluid each day. Drink steadily through the day and add electrolytes when needed.
8. Does Diamox help with Everest Base Camp altitude sickness prevention?
Diamox can help some trekkers adjust to altitude more easily and lower the risk of AMS. A doctor should advise you before you use it.
9. What should I do if I get altitude sickness symptoms on the trek?
Stop climbing right away. Rest, drink fluids, eat if possible, and tell your guide at once. If symptoms get worse, descend without delay.
10. Is a luxury Everest Base Camp trek safer for altitude sickness prevention?
A luxury Everest Base Camp trek can enhance safety by offering warm lodges, better food, stronger support from guides, daily health checks, and more reliable emergency planning. These factors help the body recover and acclimate more effectively.





